2. Ignored Evidence of Toll on Humanity due to Measures Imposed
Summary:
The data indicates that measures taken to purportedly contain the spread of COVID-19 have caused a significant negative impact at the physiological, psychological, social, political, financial, moral and ethical levels (in addition to others not listed) with the potential to impact society for generations.
- 2.1 Mental Health Consequences
- “The results indicated that anxiety score was 22.76 and 40.6% of the participant experienced moderate to severe anxiety…” (Alqudah et al., 2021)
“While COVID-19 vaccines have had a profound impact on decreasing global morbidity and mortality burdens, we argue that current population-wide mandatory vaccine policies are scientifically questionable, ethically problematic, and misguided. Such policies may lead to detrimental long-term impacts on uptake of future public health measures, including COVID-19 vaccines themselves as well as routine immunizations. Restricting people’s access to work, education, public transport, and social life based on COVID-19 vaccination status impinges on human rights, promotes stigma and social polarization, and adversely affects health and wellbeing. Mandating vaccination is one of the most powerful interventions in public health and should be used sparingly and carefully to uphold ethical norms and trust in scientific institutions. We argue that current COVID-19 vaccine policies should be reevaluated in light of negative consequences that may outweigh benefits. Leveraging empowering strategies based on trust and public consultation represent a more sustainable approach for protecting those at highest risk of COVID-19 morbidity and mortality and the health and wellbeing of the public.” (Bardosh et al., 2022)
Letter to President and Vice-Chancellor, University of British Columbia from the Office of the Chief Medical Officer, Vancouver Coastal Health (Office of the Chief Medical Officer, February 16, 2022) addressing the move towards de-registering students who have not declared their vaccination status or complied with mandatory testing stated,- “Good public health policy means implementing restrictions that are the least intrusive available, based on scientific evidence, neither arbitrary nor discriminatory in application, of limited duration, respectful of human dignity and subject to review.” [NOTE: this statement addresses well the globally ignored humanitarian aspect related to COVID-19 in the past two years].
Moreover, in regard to testing, the letter stated, “Not only is Rapid Antigen Testing of asymptomatic people unreliable in identifying infection with Omicron variant, but we have no evidence that those who have not complied with UBC policies have posed any public health risk to their fellow students, faculty or staff, even during circulation of other variants.”
“Our findings indicate a substantial proportion of students in the severe and extremely severe categories of the depression, anxiety and stress scales…Additionally, a significant proportion of students (∼50%) reported perceiving a deterioration in their mental health relative to before the onset of the COVID-19 pandemic, with the proportion of females being significantly higher than males. (Camilleri et al., 2022)
“Conclusions: Compared with a global estimated prevalence of depression of 3.44% in 2017, our pooled prevalence of 25% appears to be 7 times higher, thus suggesting an important impact of the COVID-19 outbreak on people’s mental health.” (Bueno-Notivol et al., 2021) - “Good public health policy means implementing restrictions that are the least intrusive available, based on scientific evidence, neither arbitrary nor discriminatory in application, of limited duration, respectful of human dignity and subject to review.” [NOTE: this statement addresses well the globally ignored humanitarian aspect related to COVID-19 in the past two years].
- Magnitude is difficult to currently quantify due to the typical delay that is observed in the manifestation of negative mental health consequences (Rajkumar, 2020).
- “Disease itself multiplied by forced quarantine to combat COVID-19 applied by nationwide lockdowns can produce acute panic, anxiety, obsessive behaviors, hoarding, paranoia, and depression, and post-traumatic stress disorder (PTSD) in the long run.” (Dubey et al., 2020)
- The possibility of extreme psychological stress (including data being analyzed currently from our university)…
- “Taken together, our findings support emerging research that COVID-19 can be understood as a traumatic stressor event capable of eliciting PTSD-like responses and exacerbating other related mental health problems (e.g., anxiety, depression, psychosocial functioning, etc.). Our findings add to existing literature supporting a pathogenic event memory model of traumatic stress.” (Bridgland et al., 2021) [study conducted on a sample from 5 western countries]
- “Alcohol use, PTSD, anxiety, anger, fear of contagion, perceived risk, uncertainty, and distrust are a few of the immediate and long-term effects that are likely to result from the COVID-19 pandemic.” (Esterwood and Saeed, 2020)
- “Taken together, our findings support emerging research that COVID-19 can be understood as a traumatic stressor event capable of eliciting PTSD-like responses and exacerbating other related mental health problems (e.g., anxiety, depression, psychosocial functioning, etc.). Our findings add to existing literature supporting a pathogenic event memory model of traumatic stress.” (Bridgland et al., 2021) [study conducted on a sample from 5 western countries]
- Czeisler et al. (2020)
- 40.9% of individuals reported at least one adverse event related to the pandemic:
- 30.9% depressive/anxiety disorder
- 26.3% trauma & stressor related disorder
- 13.3% started or increased substance use to cope with pandemic
- 40.9% of individuals reported at least one adverse event related to the pandemic:
- Fiorillo et al. (2020)
- “One of our main findings is the presence of moderate to severe levels of depressive, anxiety, and stress symptoms”
- “…the high rate (14.5%) of suicidal ideation/suicidal thoughts found in our sample.”
- “One of our main findings is the presence of moderate to severe levels of depressive, anxiety, and stress symptoms”
- Horigian et al. (2021)
- “Forty-nine percent of respondents reported loneliness scores above 50 [Items were summed to create a score ranging from 20 to 80, with higher scores being indicative of greater loneliness];
- 80% reported significant depressive symptoms;
- 61% reported moderate to severe anxiety;
- 30% disclosed harmful levels of drinking.
- 22% of the population reported using drugs,
- 38% reported severe drug use.
- Loneliness was associated with higher levels of mental health symptomatology. Participants reported significant increases across mental health and substance use symptoms since COVID-19”
- “Forty-nine percent of respondents reported loneliness scores above 50 [Items were summed to create a score ranging from 20 to 80, with higher scores being indicative of greater loneliness];
- “Social isolation, anxiety, fear of contagion, uncertainty, chronic stress and economic difficulties may lead to the development or exacerbation of depressive, anxiety, substance use and other psychiatric disorders in vulnerable populations including individuals with pre-existing psychiatric disorders and people who reside in high COVID-19 prevalence areas. Stress-related psychiatric conditions including mood and substance use disorders are associated with suicidal behavior. COVID-19 survivors may also be at elevated suicide risk. The COVID-19 crisis may increase suicide rates during and after the pandemic. Mental health consequences of the COVID-19 crisis including suicidal behavior are likely to be present for a long time and peak later than the actual pandemic.” (Sher, 2020)
- 25.5% (18-24yo) seriously considered suicide in 30 days prior to survey (Czeisler et al., 2020)
- The WHO itself was not consistent about the efficacy of lockdowns warning against ending them early (3/25/2020) and shortly after warning against the lockdowns due to economic damage (10/11/2020)
- “The results indicated that anxiety score was 22.76 and 40.6% of the participant experienced moderate to severe anxiety…” (Alqudah et al., 2021)
- 2.2 Drug Overdose
- 50% rise in deaths due to suspected opioid overdoses (Glober et al., 2020; Haley and Saitz, 2020; Slavova et al., 2020)
- “Synthetic opioids (primarily illicitly manufactured fentanyl) appear to be the primary driver of the increases in overdose deaths, increasing 38.4 percent from the 12-month period leading up to June 2019 compared with the 12-month period leading up to May 2020. During this time period:
- 37 of the 38 U.S. jurisdictions with available synthetic opioid data reported increases in synthetic opioid-involved overdose deaths.
- 18 of these jurisdictions reported increases greater than 50 percent.
- 10 western states reported over a 98 percent increase in synthetic opioid-involved deaths.” (CDC, 2020b)
- “The number of deaths involving alcohol increased between 2019 and 2020 (from 78927 to 99017 [relative change, 25.5%]), as did the age-adjusted rate (from 27.3 to 34.4 per 100 000 [relative change, 25.9%])…The rate increase for alcohol-related deaths in 2020 outpaced the increase in all-cause mortality, which was 16.6%. Previous reports suggest the number of opioid overdose deaths increased 38%in 2020, with a 55% increase in deaths involving synthetic opioids such as fentanyl (National Institute on Drug Abuse, 2022.) There were similar increases in the number of deaths in which alcohol contributed to overdoses of opioids (40.8%) and, specifically, synthetic opioids (59.2%). Deaths involving alcohol reflect hidden tolls of the pandemic.” (White et al., 2022)
- 50% rise in deaths due to suspected opioid overdoses (Glober et al., 2020; Haley and Saitz, 2020; Slavova et al., 2020)
- 2.3 Delays in addressing other disease
- 19-43% predicted increase in deaths due to delayed cancer surgery as a result of COVID-19 – “Modest delays in surgery for cancer incur significant impact on survival.” (Sud et al., 2020)
- Richardson and Bentley (2020) – document describes (citing other sources – see original document for citations) various aspects of disruption associated with Cancer due to COVID-19.
- Screening: “Cancer Research UK has highlighted that as a result of these measures, approximately 210,000 people per week are not being screened, thus missing the opportunity for early detection of cancer in a significant number of citizens”
- Referrals: “Amid the pandemic, urgent referrals have decreased significantly compared to usual levels in England. Early data from April by DATA-CAN, the UK Health Data Research Hub for Cancer, showed a drop as high as 76% in ‘two-week-wait’ (2WW) referrals in selected sites, while their more recent data show that this has recovered to a level that is 45% lower than normal.”
- Diagnosis: “Due to the COVID-19 outbreak, the number of performed CT scans dropped by 28% in April, May and June 2020 compared to the same time last year, with the additional challenge that CT scanning has been used to diagnose COVID-19. MRI scanning has also decreased by 53%.”
- Treatment: “Data from May shows a 29% cancellation rate of cancer surgery, equivalent to more than 36,000 surgeries, while more recent estimates suggest a reduction of up to 40%.
- Screening: “Cancer Research UK has highlighted that as a result of these measures, approximately 210,000 people per week are not being screened, thus missing the opportunity for early detection of cancer in a significant number of citizens”
- 19-43% predicted increase in deaths due to delayed cancer surgery as a result of COVID-19 – “Modest delays in surgery for cancer incur significant impact on survival.” (Sud et al., 2020)
- 2.4 Other Consequences Reported:
- 41.5% increase in pornography use in the US (Pornhub Insights, 2020)
- 8.7-30% increase in unemployment rates (Janaskie and Earle, 2020)
- 27.6-34.0% reduction in GDP across the various regions in the US (Janaskie and Earle, 2020)
- “We find that children born during the pandemic have significantly reduced verbal, motor, and overall cognitive performance compared to children born pre-pandemic. Moreover, we find that males and children in lower socioeconomic families have been most affected.” (Deoni et al., 2021)
- Disturbances in sleep (Fiorillo et al., 2020)
- “Participants reported several disturbances in sleep quality and patterns, as already found in other studies carried out in China and in other European countries” (Mandelkorn et al., 2021; Morin and Carrier, 2021).
- “Participants reported several disturbances in sleep quality and patterns, as already found in other studies carried out in China and in other European countries” (Mandelkorn et al., 2021; Morin and Carrier, 2021).
- Higher death rates in intubated patients (Richardson et al., 2020)
- “Mortality rates for those who received mechanical ventilation in the 18-to-65 and older-than-65 age groups were 76.4% and 97.2%, respectively. Mortality rates for those in the 18-to-65 and older-than-65 age groups who did not receive mechanical ventilation were 1.98% and 26.6%, respectively. There were no deaths in the younger-than-18 age group.”
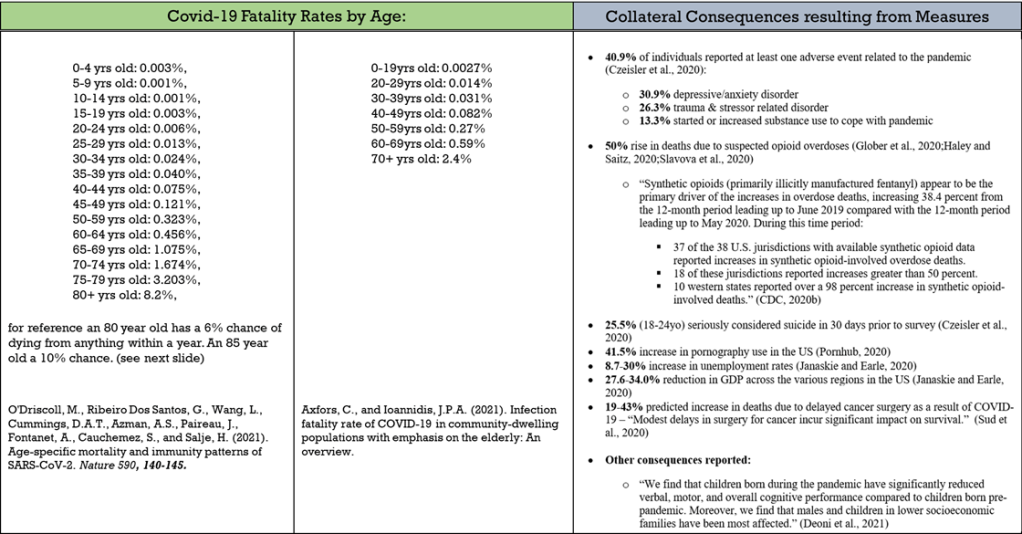
Table 2: Combined information from section 1 & 2 for comparison